Glaucoma Filtration Surgery
What is Glaucoma?
Glaucoma is one of the leading causes of blindness for people over the age of 60. Based on the WHO estimation, glaucoma patients would reach 80 million worldwide by 2020. One-third of these, primarily in Asia, are closed-angle glaucoma patients.
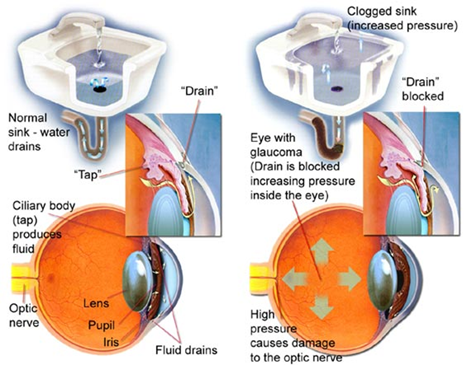
Glaucoma is a group of eye conditions that damage the optic nerve. This damage is often caused by an abnormally high pressure in the eye in hypertensive glaucoma patients. Hypertensive glaucoma is roughly divided into open-angle glaucoma and closed-angle glaucoma. Open-angle glaucoma occurs when the drainage angle formed by the cornea and iris remains open, but the trabecular meshwork is partially blocked. This causes pressure in the eye to gradually increase. This pressure damages the optic nerve. Closed-angle glaucoma occurs when the iris bulges forward to narrow or block the drainage angle formed by the cornea and iris. As a result, fluid can’t circulate through the eye and pressure increases.
Current Treatment
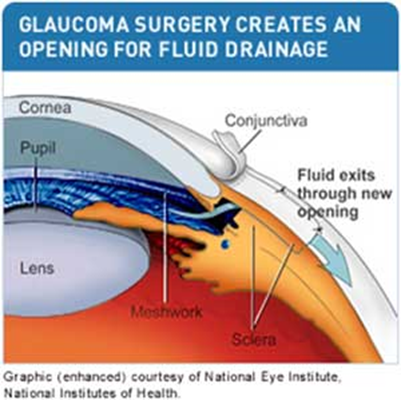
Open-angle glaucoma is treated with drug therapy and closed-angle glaucoma often requires trabeculectomy. During trabeculectomy—sometimes also called filtration surgery—a piece of tissue in the drainage angle of the eye is removed, creating an opening. The opening is partially covered with a flap of tissue from the sclera, the white part of the eye, and the conjunctiva, the clear thin covering over the sclera. This new opening allows fluid (aqueous humour) to drain out of the eye, bypassing the clogged drainage channels of the trabecular meshwork.
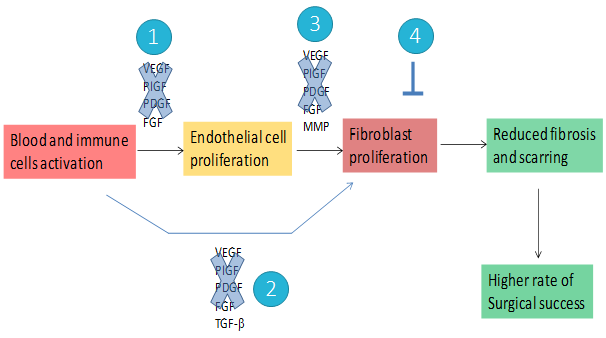
However, excess scarring and fibrosis after surgery can lead to blockage of the drainage and cause failure of GFS over time. The failures are mainly due to excessive postoperative wound healing with subsequent fibrosis and scar formation that obstruct drainage. The damage to tissue by surgery induces pro-inflammatory and pro-fibrogenic factors that can lead to abnormal extracellular matrix change and fibrosis. Myofibroblast hyper-proliferation induced by these factors subsequently causes excessive fibrosis and scar formation.
The antimetabolite drug, Mitomycin C (MMC) has been administered during glaucoma surgery as an anti-scarring agent. Another antimetabolite drug, 5-fluorouracil (5-FU), is also used mainly by local injection during follow-up. These antimetabolite drugs work by killing fast-proliferating cells involved in fibrosis. Since their activities are not selective, they can cause many side effects. For example, the anti-cell division activity sometimes causes bleb leakage post-surgery. Selectively targeted and safer postoperative management of glaucoma surgery is needed.
Cloudbreak Solution
The new drug developed by our company targets factors involved in wound healing and fibrosis. It has the potential to slow down fibrosis and scarring at the surgical site and improve the success rate of glaucoma filtration surgery.